Would you marry a woman with PCOS/hirsutism?
Houston Endocrine Center2023-05-04T15:22:30+00:00Are you a man who wants to marry a woman with PCOS/hirsutism? Does she want to marry you? Then this article is for you. I’m going to cover what PCOS/hirsutism are, how common they are, and whether they can be treated or cured. Most importantly, I’ll answer the question: will PCOS/hirsutism affect your marriage?
What is PCOS?
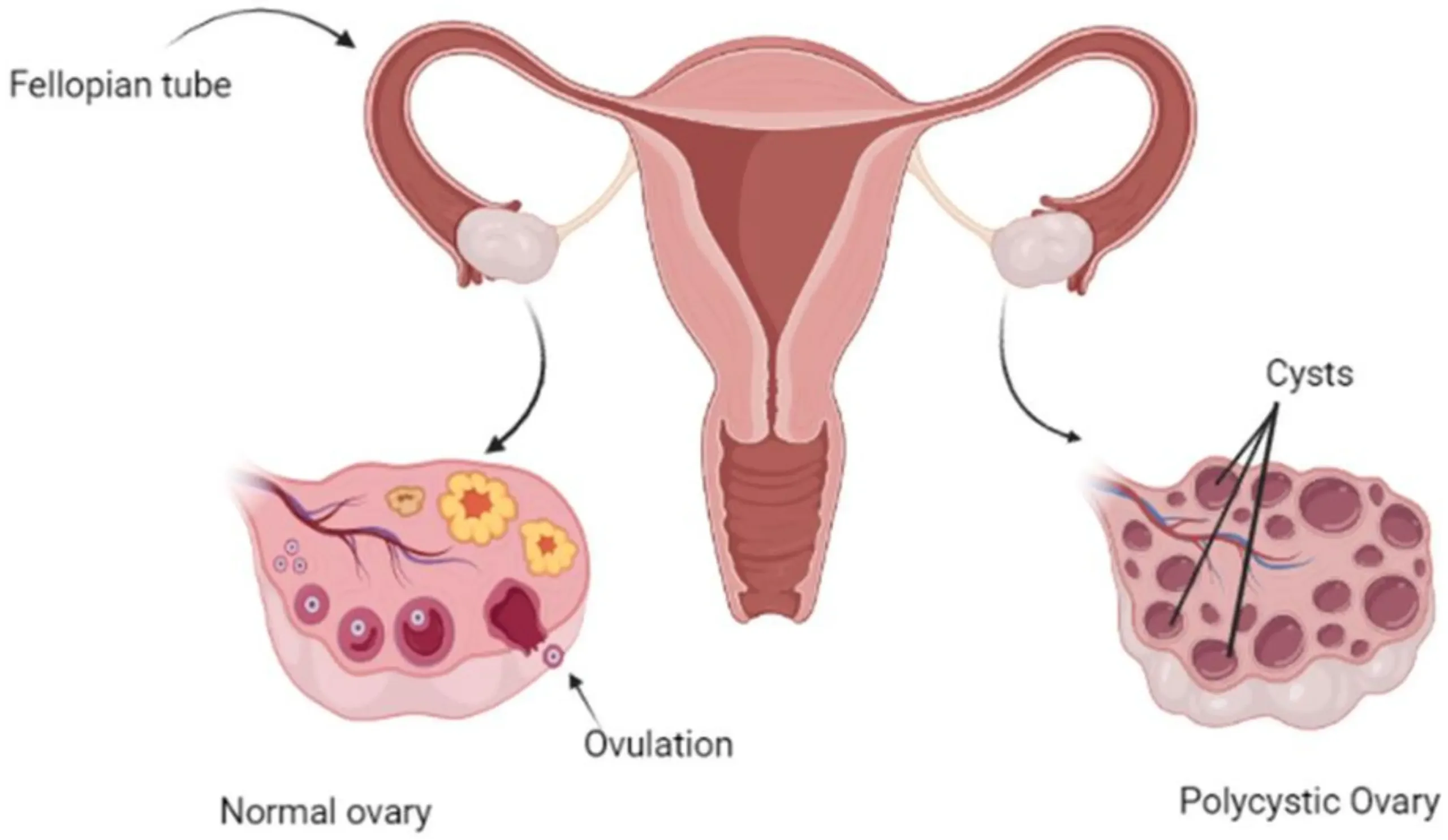
PCOS is a disorder that affects the menstrual cycle and causes ovulation to become irregular or stop altogether. Women with PCOS may also have cysts on their ovaries, high levels of male hormones (androgens) in their blood and hair growth on their face and body.
The symptoms of PCOS vary from woman to woman but can include:
- Irregular periods, which usually result in delayed or absent ovulation (the release of an egg from an ovary)
- Excessive hair growth on the face and body (hirsutism)
- Weight gain around the abdomen
If you have any of these symptoms, talk with your doctor about whether they could be due to PCOS. Your doctor may refer you for tests such as blood tests or ultrasound scans so they can diagnose whether or not you have it.
Is PCOS a real disease?
PCOS is a real disease. It’s a hormonal disorder that affects the ovaries and can cause infertility, acne, facial hair growth and weight gain. You may have heard of PCOS as “polycystic ovarian syndrome” or “polycystic ovary syndrome.”
While some women with PCOS are able to get pregnant without treatment, they may need help from their doctors if they want to become pregnant or avoid future health problems associated with PCOS (like diabetes).
How common is PCOS/hirsutism?
You may be wondering how common PCOS is. The answer depends on the source. According to the National Institutes of Health (NIH), 1 in 10 women in the United States have PCOS, which is more common in women of South Asian and Middle Eastern descent than other ethnicities. If you have a family history of PCOS and are overweight or obese, you are more likely to develop this condition as well.
What causes PCOS/hirsutism?
PCOS is a hormonal disorder that affects women in their reproductive years. The main cause of PCOS is an imbalance between the hormones estrogen and progesterone. This imbalance leads to an increase in male hormones (androgens), which causes characteristic symptoms like acne, excess hair growth on your face or body, and irregular periods.
Insulin resistance is often considered the main cause of PCOS because it leads to high blood sugar levels that can trigger problems with ovulation and fertility issues. Insulin resistance often goes hand-in-hand with other health problems such as obesity or high blood pressure–both risk factors for developing type 2 diabetes mellitus (T2DM).
Is there a cure for hirsutism?
There is no cure for PCOS. Hirsutism is a symptom of the condition and can be managed, but not cured.
In some cases, hirsutism responds favorably to medication and/or laser hair removal. However, it may take several months or even years before you start to see results.
What are the symptoms of PCOS/hirsutism in men and women?
The symptoms of PCOS/hirsutism in men and women include:
- menstrual irregularities
- acne
- weight gain
- hair growth on the face, chest, stomach and back (for women) or chest and back (for men)
In addition to these symptoms, women with PCOS may also experience infertility as well as high blood pressure or heart disease. Men who have it can develop diabetes.
Is it possible to identify who has PCOS or hirsutism early on?
Yes, it is possible to identify who has PCOS or hirsutism early on. Early detection of these conditions is important because it can help prevent serious health problems later in life.
How can you tell if someone has PCOS?
There are several symptoms that may indicate that you have PCOS:
- Irregular periods (or no periods)
- Excessive hair growth on the face and body, called hirsutism
- Acne or oily skin
Can pregnancy help reduce the symptoms of hirsutism?
Pregnancy can cause hirsutism to get worse.
The cause of hirsutism is often an imbalance in hormone levels, and pregnancy can disrupt this balance even more. In addition, as your body changes during pregnancy, it may trigger more hair growth than usual.
What are the effects of PCOS on marriage?
The effects of PCOS on marriage are far-reaching and can have a serious impact on your relationship. Some of the most common issues include:
- Infertility.
Women with PCOS have difficulty getting pregnant, which can make it difficult for couples to start a family. If you’re not ready to start a family yet, this may not be an issue for you–but if you want children someday and can’t conceive naturally because of your partner’s condition, then this could pose some serious problems down the line.
- Irregular menstrual cycles or polycystic ovaries (PCO).
Many women experience irregular menstrual cycles during their adolescence due to hormonal imbalances caused by PCOS symptoms like acne or excess body hair growth; this makes tracking ovulation difficult and increases risk for pregnancy complications such as miscarriage or preterm labor if intercourse occurs during an infertile period.* Increased risk for Type 2 diabetes mellitus (T2DM) as well as cardiovascular disease (CVD). Both conditions are associated with greater mortality rates among people living with them than those without these diseases.*
Conclusion
After reading this article, you should have a better understanding of what PCOS and hirsutism are. You may also be wondering if it’s possible to marry a woman with these conditions. The answer is yes! If both partners are willing to work together and find solutions for their individual needs, then they can build a strong relationship that lasts forever.