Source: Pinterest
The thyroid and parathyroid are two small glands that help control your metabolism, body temperature, and the rate of protein synthesis. They also produce hormones that regulate how your body uses energy and the calcium in your bones.
Several diseases are related to these glands, including hyperthyroidism, hypothyroidism, and thyroiditis.
The parathyroid produces the hormone parathormone, and the thyroid produces the hormones thyroxine and triiodothyronine. These hormones are produced from iodine, which is a mineral that your body needs. The thyroid gland will dump out more iodine when it’s low on calcium, so it makes sense that an imbalance of iodine and calcium could lead to hypothyroidism.
There are many more things you need to know about the working of the thyroid and parathyroid glands. If you want to learn more on this topic, keep reading this blog.
What Is The Thyroid?
The thyroid gland is a small, butterfly-shaped gland. The thyroid is an essential part of the endocrine system and plays an important role in maintaining normal body function. It was discovered in 1873 by French physician Emile-Jean Démeunier. He observed a lump on a patient’s neck with goiter and found it attached to the front of the trachea. Démeunier decided the lump was a gland and called it the “glandula thyreoidea”. In most people, this gland is just below the larynx.
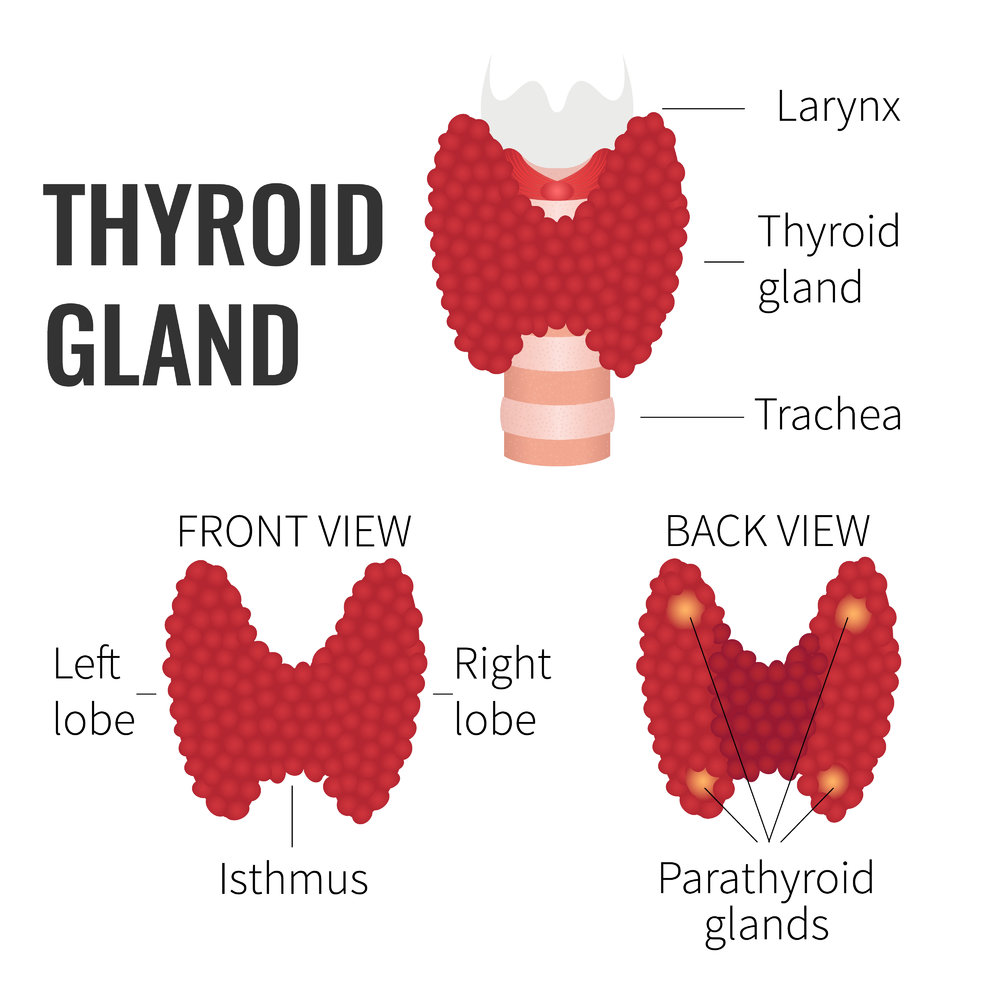
Source: Getty Images
The thyroid produces a hormone called thyroxine that helps regulate metabolism, growth, and the body’s use of energy. It is also responsible for regulating body temperature, growth, development, and sexual maturation. It also helps in influencing heart rate, blood pressure, and breathing.
There is less metabolic activity when your thyroid is not producing enough thyroxine. This can lead to weight gain, a bloated feeling in your body due to bloating the stomach and intestines with gas bubbles increasing in size and number over time, fatigue, weight loss, or decreased appetite.
Where Is The Thyroid Gland
The thyroid gland is located in front of the windpipe in the neck, near where the larynx joins it. It produces hormones that help regulate the rate of protein synthesis in your body, which is important for muscle growth and repair. It produces two hormones secreted into a small canal (the laryngeal lumen) connecting to the lungs and blood vessels on the other side.

Source: Shutter Stock
Thyroid Functions
Thyroid functions are how thyroids produce and regulate hormones. There are three main types of thyroid functions:
- Iodine-dependent thyroid function
- Iodine-independent thyroid function
- Thyroid autoimmunity.
Iodine-Dependent Thyroid Functions
Iodine-dependent thyroid functions rely on the presence of iodine to regulate hormones. These thyroids use either iodide or iodate, stored in the body’s cells, to regulate hormone production, release, and function. Iodide is more commonly used as it is less toxic for the body, but iodate has a higher capacity for regulating hormones.
Iodine-Independent Thyroid Functions
Iodine-independent thyroid functions use proteins called thyroid peroxidase to produce thyroxine (T4) and triiodothyronine (T3) without the need for iodine. Thyroid peroxidase is produced by the thyroid cells.
Thyroid Autoimmunity
Thyroid autoimmunity has no known cause, but it is characterized by an overreaction of the immune system against thyroids. The immune system reacts at a cellular level and attacks the thyroid, resulting in an inability to produce hormones or an inability to regulate hormone production.
How Does Thyroid Work?
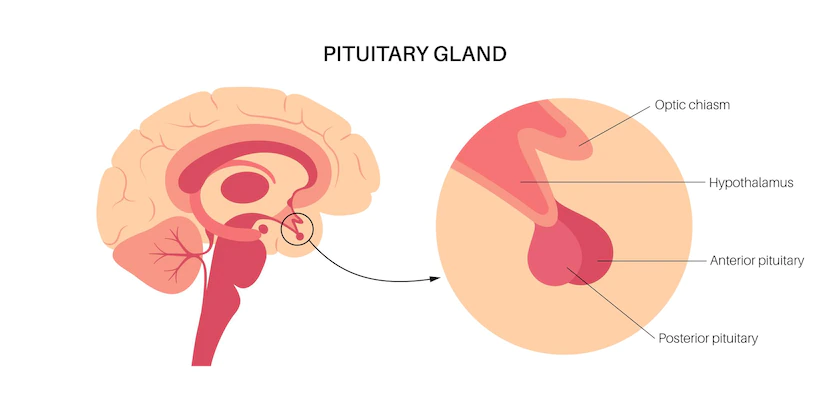
The thyroid is controlled by a hormone called Thyrotropin-Releasing Hormone (TRH). This hormone is released from the hypothalamus, located deep in the brain. The TRH then stimulates cells in the pituitary gland to release thyroxine and triiodothyronine. These hormones then stimulate the thyroid to increase or decrease the production of two hormones:
- Thyroxine (T4)
- Triiodothyronine (T3).
T4 is converted to T3, regulating how much energy you burn. T3 is then transported around the body and used for energy. The conversion rate from T4 to T3 varies among individuals, which can often be corrected by medications (such as lithium).
When you are cold, your body uses more energy to keep warm, and this causes T3 levels to decrease. The T3 level must be high to maintain normal body temperature and function.
Lack of sleep causes a low T3 level and, ultimately, a low metabolic rate. Take one or two fish oil capsules (500 mg) daily to maintain healthy energy levels and metabolism during sleep deprivation.
The thyroid gland also helps regulate your moods, sleep patterns, body temperature, etc.
What Is The Parathyroid?
The parathyroid is a small gland that sits on top of the thyroid gland. It is responsible for controlling calcium levels in the blood. When the parathyroid is functioning properly, calcium levels stay within a normal range.

Source: Freepik
The parathyroid gland makes up about 2% of total body weight and is located in the neck near the thyroid gland. The parathyroid can be found in two different shapes – spherical and tubular. The shape of the parathyroid can tell you whether it is functioning properly or not. If the parathyroid is not functioning properly, calcium levels are likely elevated.
Generally, the parathyroid gland comprises four small glands called “cores” in a spherical shape and two tubular “arms.” The most common cause of hyperparathyroidism is a tumor on one or more glands.
Parathyroid cancer is rare and has an incidence rate of about 1 in 500,000 people per year. An alteration in the parathyroid genes (mutations) can lead to the overproduction of the parathyroid hormone.
Where Is The Parathyroid Gland
The parathyroid is found on either side of the thyroid gland near where you can feel it with a finger or two. This gland helps regulate calcium levels in your blood by controlling how much calcium you absorb from food sources or drinks. It also helps regulate how much calcium is released into your blood when needed.
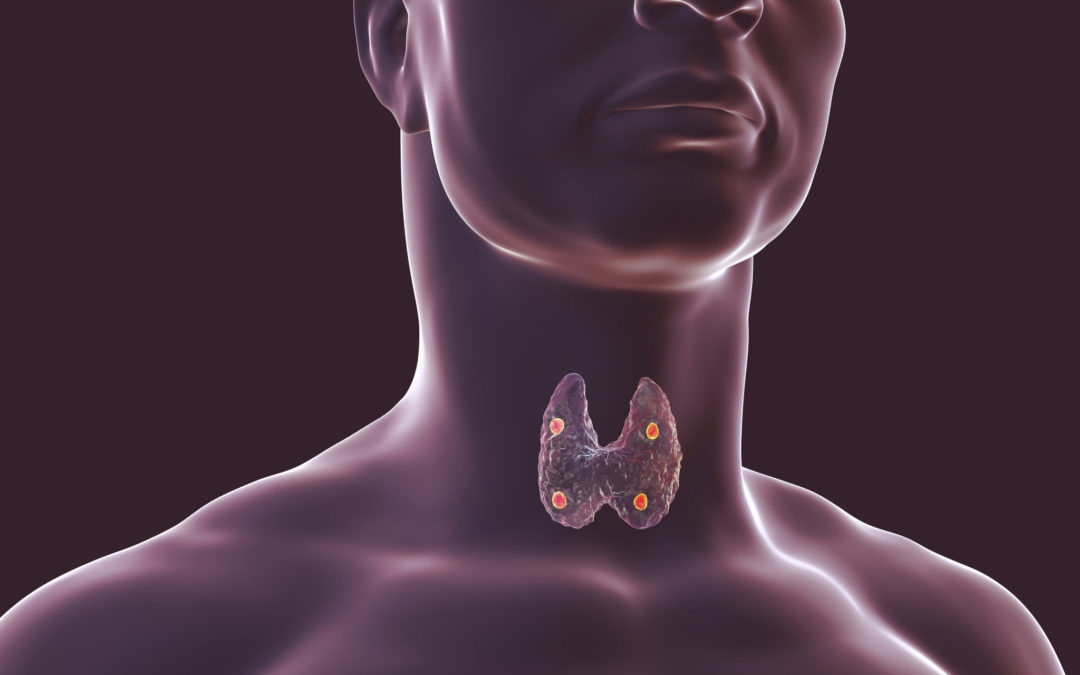
Source: Shutter Stock
Parathyroid Functions
The parathyroid glands are four small glands located near the thyroid gland on each side of your neck. The two on the left side of your neck produce parathyroid hormone, while those on the right side produce calcitonin. Both hormones help regulate calcium levels in your blood and maintain bone health.
Parathyroid functions involve four hormones:
1) Parathyroid hormone (PTH)
2) Calcitonin
3) Thyroxine
4) Thyrotropin-releasing hormone (TRH)
Parathyroid Hormone (PTH)
PTH is a hormone that helps regulate calcium levels in the blood, providing the feedback mechanism to keep calcium and phosphorus levels in balance. It is also involved in bone growth and metabolism regulation.
Calcitonin
Calcitonin is a hormone that helps maintain bone health by inhibiting osteoclasts, cells that break down the bone matrix while promoting osteoblasts, cells that build the bone matrix. It also inhibits bone resorption.
Thyroxine
Thyroxine is a hormone that regulates metabolism and growth by stimulating the thyroid gland to produce and release more of its hormone, thyroxine. TRH is a stimulant of the pituitary gland that regulates thyroid function by stimulating, in turn, the production of thyrotropin, which is the major thyroid hormone.
Thyrotropin-Releasing Hormone (TRH)
The function of the parathyroid is to regulate calcium levels in the blood by releasing more or less hormone into it when needed. Low calcium levels release more hormones into your system, increasing your blood calcium level and making you feel more energetic or alert than usual.
How Does Parathyroid Work?
The parathyroid helps regulate calcium and vitamin D levels in the blood. This gland secretes parathyroid hormone (PTH) into your bloodstream, which helps regulate these levels by increasing calcium absorption from food. PTH helps maintain the right calcium level in the blood by telling the kidneys how much to excrete and how much to conserve.

Source: Freepik
The effect of PTH is the opposite in diabetics, an adrenal gland tumor, hyperparathyroidism, or other diseases that cause hypercalcemia. If a parathyroid gland tumor is found in the neck, it is often surgically removed.
The parathyroid gland is also known as the “master gland” because it controls many other hormones, including calcitonin, phosphorus, and thyroid-stimulating hormone. This gland is also responsible for regulating the body’s calcium levels, and it does so by leaching calcium from the bones.
How Are The Thyroid And Parathyroid Related?
The thyroid and parathyroid are both glands that produce hormones. The thyroid produces thyroxine, which is responsible for the production of metabolic rate and energy by controlling how much energy, or calories, we need to produce.
On the other hand, the parathyroid produces a hormone (PTH) responsible for regulating how much calcium is absorbed and helps the body maintain a proper calcium level in the blood. There are two types of parathyroid glands:
- The superior
- The inferior
The superior is located at the top of the thyroid gland, while the inferior is located on its side. Both glands regulate calcium levels in your bloodstream to help support bone and muscle health.

Source: Pinterest
The thyroid and parathyroid are important glands in our body that work together to regulate our metabolism. The hormones produced by these glands can help regulate what happens to our bodies and other glands like ovaries and testes. It can cause many health complications such as hypothyroidism or hyperparathyroidism when one is not functioning normally.
The most common thyroid and parathyroid-related health condition that people struggle with is hypothyroidism. There isn’t enough thyroxine in the body in hypothyroidism to function properly. This can be caused by genetics or lifestyle factors such as stress or diet choices.
Disorders Of Thyroid Glands
A condition in which the thyroid produces more or less hormone than the body needs. Thyroid disorders are the most common endocrine diseases in the world. They are characterized by hyperfunction or hypofunction of the thyroid gland.

Source:Shutter Stock
Hyperthyroidism, also known as thyrotoxicosis, is characterized by excessive production of thyroxine (T4) and triiodothyronine (T3) by the thyroid gland causing an increase in metabolic rate and heart rate, increased perspiration, heat intolerance, and weight loss. A condition in which the thyroid produces less hormone than the body needs.
Hypothyroidism, also known as thyrotoxicosis, is characterized by insufficient production of thyroxine (T4) and triiodothyronine (T3) by the thyroid gland causing a reduced metabolic rate and heart rate, weight gain, and increasing difficulty concentrating.
Thyroid disorders are classified into six types:
- Thyrotoxicosis,
- Hyperthyroidism,
- Hypothyroidism,
- Multinodular goiter,
- Graves’ disease, and
- Hashimoto’s thyroiditis.
Thyrotoxicosis
Thyrotoxicosis is caused by the overexertion of the thyroid gland, which produces excessive amounts of thyroid hormone. Results include hyperthyroidism with symptoms such as palpitations and heat intolerance.
Hyperthyroidism
Hyperthyroidism is when the thyroid gland produces too much thyroid hormone. The symptoms of hyperthyroidism include rapid or irregular heart rate, weight loss, anxiety, palpitations, and tremors.
Hypothyroidism
Hypothyroidism is a type I and type II in which the thyroid gland does not produce enough hormones. In hypothyroidism, symptoms may include weight gain, fatigue, feeling cold all the time, constipation, dry skin and hair.

Multinodular Goiter
Multinodular goiter is an enlarged thyroid gland with a collection of multiple nodules within it. An enlarged thyroid gland is a multinodular goiter’s most common sign and symptom. The cause of multinodular goiter is unknown. Some people with this type of thyroid gland have a genetic mutation that may cause the development of multinodular goiters.
Graves’ Disease
Graves’ disease is a condition that causes the thyroid to produce too much thyroid hormone. This hormone is produced by the body and regulates how fast our metabolism works. It also helps control how much energy we have, how well our organs, muscles, and bones function, and how quickly we grow.
Hashimoto’s Thyroiditis
Hashimoto’s thyroiditis is an autoimmune disorder that involves antibodies attacking the gland. In Hashimoto’s disorder, symptoms may include an enlarged thyroid gland, chronic fatigue syndrome, and pain in the front of the neck.
What Are The Symptoms Of Thyroid Disorders?
There are a few symptoms of thyroid disorders that are hard to miss. They include:
- Fatigue
- Weight gain
- Skin creases around the neck (trachea)
- Dry skin
- Dry hair
- Constipation
- Muscle weakness
- Muscle pain
- Joint pain
- Depression
- Weight loss
- Hoarseness
- Sleep apnea
- Swelling in the neck
- Enlarged lymph nodes in the neck
- Difficulty breathing
- Difficulty talking
- A change in voice pitch when trying to talk
Thyroid disorders can be diagnosed based on the physical symptoms that a person experiences. However, some tests can detect thyroid problems before they become severe.
Disorders Of Parathyroid Gland
The parathyroid gland is located in the neck. It is responsible for controlling the amount of calcium and phosphate in your blood. It also regulates how much thyroxine and calcitriol are released into the bloodstream.
Parathyroid gland disorders can be caused by various factors, including genetic, environmental, or an autoimmune response to a virus or bacteria. There are four types of parathyroid disorders:
- Hyperparathyroidism
- Hypoparathyroidism
- Primary hyperparathyroidism
- Secondary hyperparathyroidism
Hyperparathyroidism
Hyperparathyroidism is caused by an overproduction of parathyroid hormone and is typically associated with metabolic syndrome.
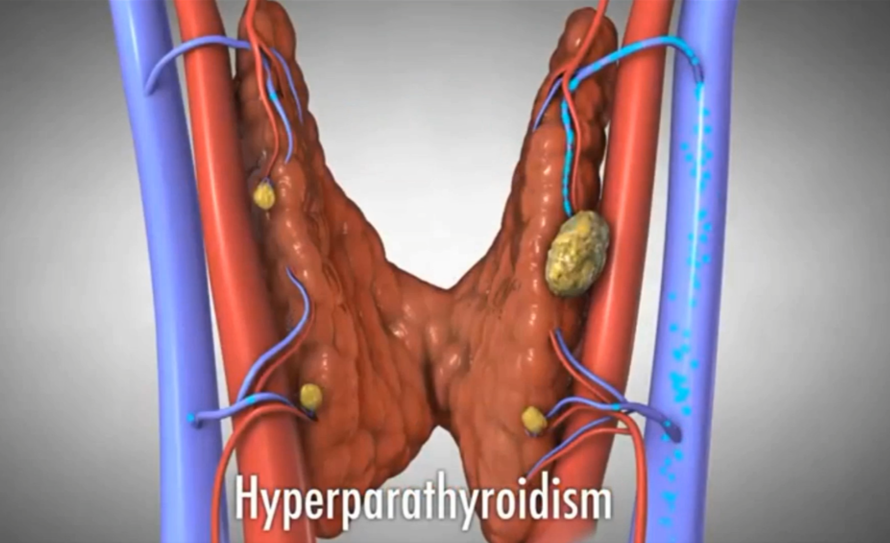
Source: Rise Surgical
Hypoparathyroidism
Hypoparathyroidism occurs when there is a deficiency in parathyroid hormone, which can happen after surgical removal or destruction of each parathyroid gland.
Primary Hyperparathyroidism
Primary hyperparathyroidism requires no cause and follows the same course as secondary hyperparathyroidism.
Secondary Hyperparathyroidism
Secondary hyperparathyroidism is caused by damage or inflammation of the parathyroid glands, which can be caused by various factors like a disease process in nearby organs, surgery to remove a tumor, or damage from radiation therapy.
What Are The Symptoms Of Parathyroid Disorders?
The symptoms of Parathyroid disorders may vary depending on the type of disorder and the severity. Some common symptoms include:
- Muscle cramps
- Pain in the neck
- Back, shoulders, or arms pain
- Frequent urination
- Severe fatigue
- Unexplained weight loss
- Hair loss
- Changes in skin color
- Blurred vision
- Dry mouth
- Nausea
- Vomiting
- Severe constipation
- Irritability
- Dizziness
- High blood pressure
- Low potassium levels
The most common cause of hyperparathyroidism is a tumor on the parathyroid gland. Other causes include:
- Genetic defects.
- Damage to the parathyroid glands from radiation.
- Overproduction of parathyroid hormone by the pituitary gland.
The Importance Of Maintaining A Healthy Thyroid And Parathyroid
The thyroid and parathyroid glands are responsible for producing hormones that control metabolism, growth, and body temperature.
There is an increasing number of people suffering from thyroid or parathyroid problems due to various factors such as aging, genetics, and environmental pollutants. It is important to know how to maintain a healthy thyroid and parathyroid gland to live a long life with good health.

Source: Freepik
Maintaining a healthy thyroid and parathyroid gland cannot be overemphasized, especially when facing a problem with one or more of these glands. In the last ten years, the number of people undergoing medical treatment for thyroid problems has increased due to various factors such as aging and environmental pollutants. More people are now maintaining healthy thyroid by taking proper care through diet, lifestyle changes, and medication.
Here we discuss natural ways to maintain a healthy thyroid and parathyroid gland:
- Consume foods that are rich in iodine, like seafood and seaweed. Iodine is a chemical element necessary for the normal functioning of the thyroid gland. It helps synthesize hormones like T3, T4, and calcitonin involved in the metabolism of cells, oxygen utilization, and heat production by the body.
- Consume foods that are rich in calcium and magnesium like chia, lime, and tofu. The body only absorbs 60% of what it needs from food sources, so other requirements must be met through diet to maintain a healthy thyroid and parathyroid gland.
- Consume foods rich in vitamins B12 and D. The thyroid and parathyroid gland cannot produce these vitamins independently, so they must be obtained through dietary sources. In general, vitamin D is produced by the body when exposed to sunlight, while vitamin B12 is found in animal products like meat, dairy, eggs, and fish.
- Consume a mineral-rich diet. The thyroid releases hormones that regulate metabolism and energy levels. When the thyroid isn’t properly functioning or functioning at a low level, it can lead to hypothyroidism which consists of many symptoms including fatigue, dry skin, cold intolerance, weight gain, hair loss, and constipation.
- Consuming antioxidants found in fruits and vegetables like strawberries, blueberries, and kale can help protect the thyroid from oxidative stress.
- Consuming foods high in niacin like eggs, meat, poultry, and fish can help the thyroid function properly.
- Consuming fats doesn’t affect the function of the thyroid.
- One of the best foods to help maintain good thyroid function is a diet rich in whole grains, nuts, and seeds.
When these glands become underactive or overactive, they can lead to various health problems such as hypothyroidism or hyperthyroidism.