How Would You Differentiate Between Osteoporosis And Arthritis?
Houston Endocrine Center2022-09-28T14:38:26+00:00Osteoporosis and arthritis are two health conditions that can be difficult to diagnose because they share some of the same symptoms. Some of these include joint pain, loss of mobility, and limited or painful movement. If you have ever had either one or both, you know how unpleasant and painful it can be. If you have not had them before, or your family members have not had either one, you might be wondering how doctors differentiate between osteoporosis and arthritis.
Source: VectorStock
We will show you some differences that can help you differentiate between osteoporosis and arthritis. We will also describe each condition in detail, along with their types. Let us get started.
What Is Osteoporosis?
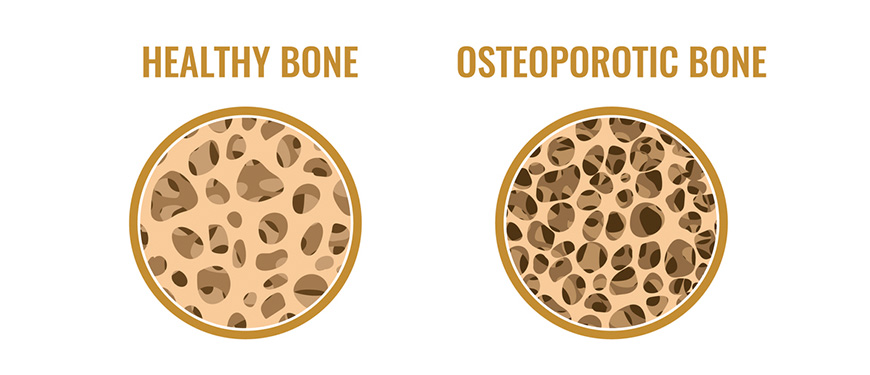
Osteoporosis is a disease in which the bones become thin and weak and break easily. This can happen after age 50, but it is more common in older women than men.
Older people are at greater risk because as we age, our bones naturally begin to lose calcium and other minerals. Osteoporosis causes this loss of minerals to increase at an abnormal rate. Over time, bones become increasingly fragile and break easily.

Source: VectorStock
Osteoporosis affects more than 10 million Americans — mostly older women — and accounts for about 1 in 5 fractures in American adults age 65 or older. More than 80 percent of all hip fractures result from osteoporosis or low bone mass, according to the National Osteoporosis Foundation (NOF). The NOF estimates that an additional 200,000 Americans will suffer hip fractures this year due to osteoporosis.
What Are The Types Of Osteoporosis?
Osteoporosis is a common condition that primarily affects older people, but it can also affect younger people who have certain medical conditions. There are two main types of osteoporosis: primary and secondary.
Primary Osteoporosis
Primary osteoporosis occurs when your body does not make enough new bone as you grow older. This type of osteoporosis is also known as senile osteoporosis or senile osteopenia. It’s more common among older men than women, and it is not life-threatening if you catch it early enough and take steps to prevent fractures.
Secondary Osteoporosis
Secondary osteoporosis occurs when there are other problems with your body that affect your bones. Some examples of secondary osteoporosis include Paget’s disease, hyperparathyroidism, and kidney failure (renal osteodystrophy). Secondary osteoporosis can be life-threatening if you do not get treatment right away.

Source: VectorStock
Menopausal osteoporosis is also a common type of osteoporosis.
Menopausal Osteoporosis
Menopausal osteoporosis is characterized by bone loss that occurs as a result of menopause. It can lead to bone fractures, which can be painful and debilitating. The most common type of menopausal osteoporosis is postmenopausal osteoporosis (PMO), which occurs after the last menstrual period. The condition may also be called climacteric osteoporosis or senile osteoporosis.
Menopausal osteoporosis occurs when the body stops producing estrogen and progesterone, which are hormones that help maintain bone density. Without these hormones, the bones become fragile and more likely to fracture from a minor fall or other injuries. Menstruating women lose an average of 0.5% of their bone density each year until menopause, when bone loss accelerates between ages 40 and 60 years old.
What Is Arthritis?
Arthritis is a disease in which your joints — the places where two or more bones meet — become inflamed and swollen. The inflammation makes the joints stiff and painful. It occurs when a person’s joints are damaged, and the lubricating fluid that helps them move becomes less effective. Arthritis can be caused by injury, infection, or overuse of a joint. It can also be genetic (inherited), or it may occur when you are older.

Source: VectorStock
Arthritis is not contagious or caused by any one thing. You can’t catch it from someone else or give it to someone else. Arthritis results from damage to your joints that make it hard for them to move smoothly against each other without causing pain. Arthritis can affect any joint in your body, including your fingers, hands, wrists, hips, knees, ankles, and feet. It can also affect other connective tissues throughout your body like tendons, ligaments, and even muscles.
Arthritis is not just one disease; it’s actually an umbrella term for several types of joint problems that cause similar symptoms and are treated with similar therapies. Over time, people with arthritis may develop deformities such as bony spurs (small growths) on their joints as well as bone weakness and/or loss of cartilage (the hard tissue that covers the ends of bones).
What Are The Types Of Arthritis?
There are many types of arthritis. The most common types are osteoarthritis (OA) and rheumatoid arthritis (RA). Most cases of arthritis are osteoarthritis.
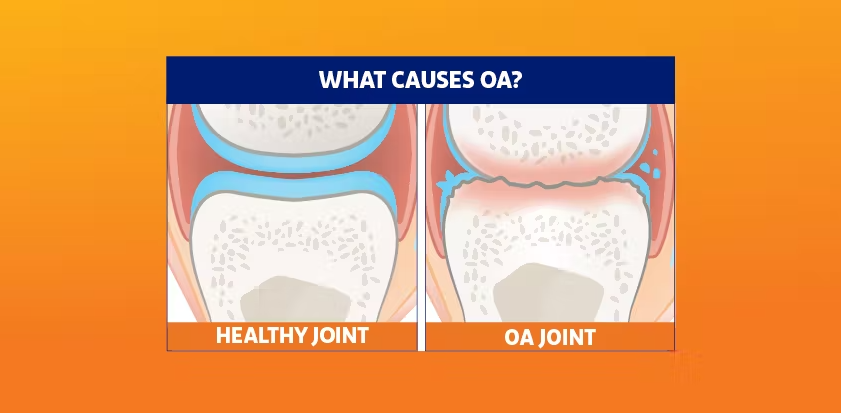
Osteoarthritis
Osteoarthritis occurs when the cartilage within the joints wears away over time. Cartilage is a rubbery tissue that cushions bones where they meet at the ends of bones in a joint. It also helps with movement by allowing smooth gliding between bones. When cartilage breaks down, it causes pain and stiffness in a joint because bones can rub together more easily. Osteoarthritis usually develops gradually over time as a result of aging or injury.

Source: VectorStock
Rheumatoid Arthritis
Rheumatoid arthritis is a chronic disease that causes pain, swelling, and stiffness in your joints. It also can affect other parts of your body, especially the skin, eyes, and lungs. The cause of rheumatoid arthritis isn’t known, but it most often develops after age 40. Women are affected more often than men.
Rheumatoid arthritis usually causes joint pain that is symmetrical — meaning it occurs on both sides of the body — although some people may have asymmetrical symptoms. Symptoms can range from mild to severe and last for weeks or months at a time before improving or worsening again.
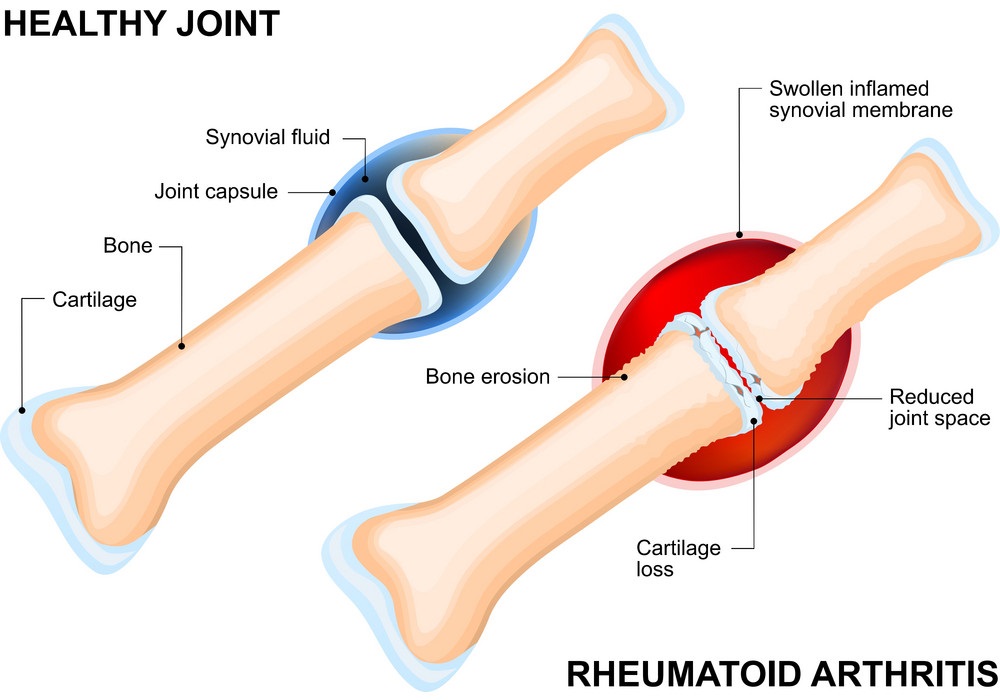
Source: VectorStock
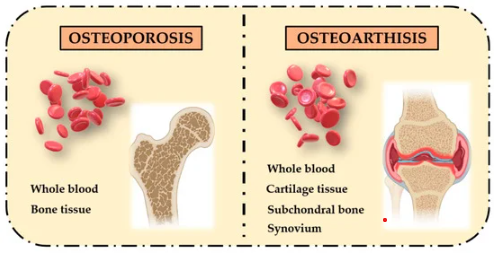
What Are The Differences Between Osteoporosis And Arthritis?
Osteoporosis and arthritis are two different kinds of diseases. Although they share some common characteristics, there are some major differences between the two conditions that make them very different from each other.

Source: VectorStock
| Osteoporosis | Arthritis |
|---|---|
| Osteoporosis is a disease that causes bones to become weak and fragile. The bones get thinner and can break easily, which can lead to pain and disability. | Arthritis is a group of more than 100 diseases that cause pain, swelling, stiffness, and loss of function in your joints. There are many different types of arthritis. |
| Osteoporosis is a condition that leads to the weakening of bones to the point of fracture. | Arthritis is a condition that leads to inflammation of the joints and surrounding tissues. |
| Osteoporosis affects bones primarily. | Arthritis affects joints primarily. |
| Osteoporosis can lead to fractures. | Arthritis can lead to loss of mobility and deformity. |
| Osteoporosis causes your bones to be more likely to break, often without you even knowing it. | Arthritis causes pain, swelling, and stiffness in your joints. |
| Osteoporosis can be caused by genetics, age, smoking, and more. | Arthritis can be caused by physical injury, obesity, genetics, stress, and more. |
| Osteoporosis can be treated with medications that slow its progress or even rebuild bone, but there’s no cure for the disease. | There are several types of arthritis, each with its own cause and treatment. |
| Osteoporosis usually affects older people; most people with osteoporosis are 65 or older. But osteoporosis can affect anyone at any age. | Arthritis does not just happen as you get older; it can start at any age. |
Do Osteoporosis And Arthritis Have Anything In Common?
The answer is yes! In fact, they are closely related.
Source: VectorStock
- Osteoporosis and arthritis are both chronic conditions that cause pain and disability.
- Both conditions are more common with age. Both osteoporosis and arthritis can affect people of all ages but usually occur after age 50.
- They are much more common in women than men because women have thinner bones than men do at any given age; this makes them more prone to breaking when subjected to stress or trauma.
- Both conditions can affect any joints in the body and can cause pain and decreased mobility.
- Osteoporosis occurs when the body does not produce enough new bone tissue, causing the existing bone to become brittle and weak over time. Osteoarthritis happens when cartilage (the smooth tissue that covers the ends of bones) wears down over time due to repeated stress on the joints from everyday activities such as walking or lifting objects.
- Osteoporosis and arthritis are both conditions characterized by painful, debilitating joint issues.
- Both osteoporosis and arthritis can make it difficult for people to perform daily tasks or exercise.
- While osteoporosis and arthritis are not the same, they share many symptoms, such as;
- Pain in your joints
- Swelling in your joints
- Stiffness in your joints
Conclusion & Takeaway
Osteoporosis and arthritis are two of the most common medical conditions in our country. They are both diseases that cause pain and can lead to long-term disability for those who suffer from them. The best way to treat either disease is with a combination of diet, exercise, and medication which are tailored to help alleviate your specific symptoms. Changes in lifestyle may need to be made if either disease is diagnosed. However, many people will be able to manage their osteoporosis or arthritis while still enjoying a fulfilling life.

Source: VectprStock
If you want to know more about the treatment options available for osteoporosis and arthritis, please feel free to contact us via WhatsApp at +1 832-862-3236 or visit our website to book an appointment with us.
We help people with endocrine disorders. Endocrine disorder treatments do not have to jeopardize your life. There is a better way – Houston Endocrine Center dedicates to delivering the best endocrinology care to provide patients with the quality of life they deserve.